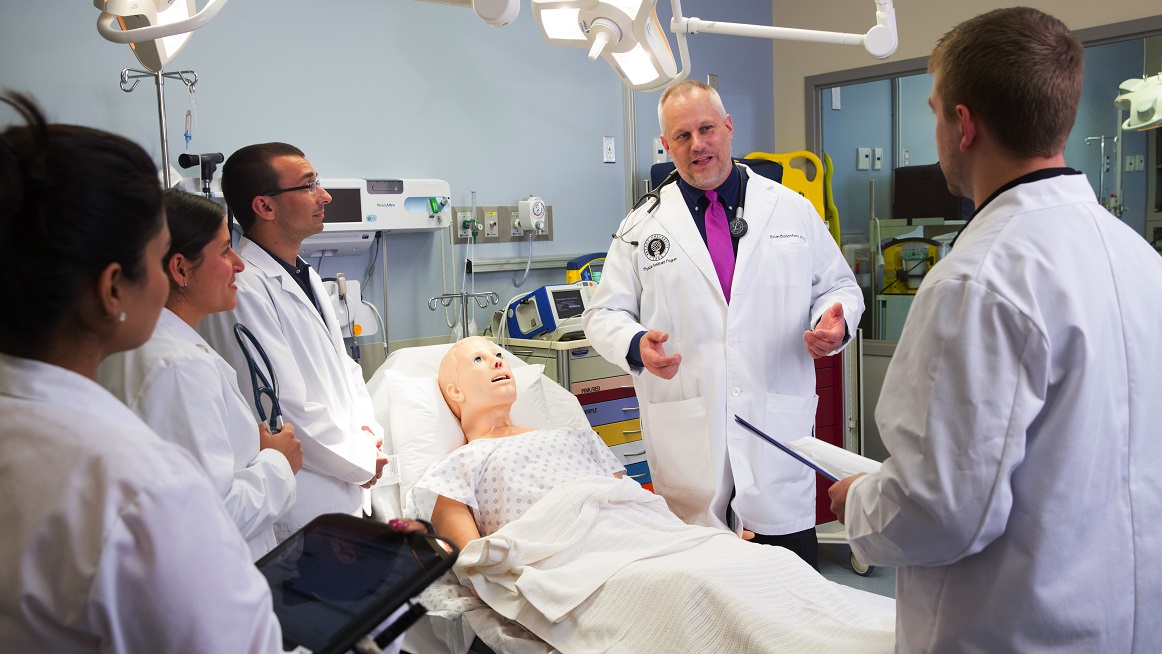
SMITHFIELD, RI - Robert Jay Amrien, MPAS, PA-C, is the founding Program Director and Clinical Associate Professor for Bryant University’s Physician Assistant program. In addition to his years of leadership, clinical, and teaching experience, he served in the U.S. Coast Guard for 22 years. He currently works as a Physician Assistant at Massachusetts General Hospital and leads a weekly student clinic at the Rhode Island Free Clinic.
 Amrien's decades of clinical experience, including treating patients during the COVID-19 crisis, combined with his administrative, leadership, and teaching experience, give him a unique perspective on this crisis and what we are learning about the U.S. healthcare. In this Q&A he shares his real-time observations from the front lines.
Amrien's decades of clinical experience, including treating patients during the COVID-19 crisis, combined with his administrative, leadership, and teaching experience, give him a unique perspective on this crisis and what we are learning about the U.S. healthcare. In this Q&A he shares his real-time observations from the front lines.
What are your overall observations about how the healthcare system is equipped to respond to COVID-19?
I don’t think anyone was prepared for an epidemic on the scale of what we are experiencing with SARS-CoV2 (COVID-19). I have been involved in healthcare for the greater part of my adult life, and I always felt prepared for anything, but this has been different.
The incident command system in the U.S. has been tested and proven to be highly effective. Large scale events like 9-11, Hurricane Katrina, and the floods in the Southwest have challenged our systems, and we have always been able to accommodate the need, albeit, often with assistance from the well-prepared Federal Government.
The difference with the COVID-19 outbreak is that it is affecting not only our entire country, but most of the world. Any backup supplies and stockpiles are being used at a rate that no one could have expected.
The difference with the COVID-19 outbreak is that it is affecting not only our entire country, but most of the world. Any backup supplies and stockpiles are being used at a rate that no one could have expected.
So far, certain states and systems have been completely overwhelmed. For example, look at New York City (NYC), Detroit, and New Orleans. Once we are beyond this crisis, we can look back at factors involved in these areas becoming hot spots, but for now we need to quickly focus on taking the lessons learned from these areas and applying prophylactic or preemptive measures in areas that are not yet as affected.
One of the most important takeaways will be a very real understanding of the shortcomings in the many interconnected systems involved in managing a global crisis. As bad as this crisis is, it might have been worse with a more virulent disease. If we learn our lessons from this event, we’ll be much better prepared for the future.
You are experiencing this pandemic through the systems in Rhode Island and Massachusetts. How is it going?
Massachusetts and Rhode Island are among the states leading the country in our response both on the civic level and as a collection of healthcare systems. We have not yet reached a surge, so we are managing fairly well, dealing with many uncertainties as information changes by the hour.
[Everyone is] coming together with an unseen resolve and tremendous bravery to fight this virus despite great risk to themselves and their loved ones.
What I am seeing, and I feel is critical to convey, is that there is tremendous dedication among our healthcare providers. I have seen doctors, PAs, nurses, technicians, respiratory therapists, radiologic technologists, sonographers, interpreters, scribes, and everyone else coming together with an unseen resolve and tremendous bravery to fight this virus despite great risk to themselves and their loved ones. I have not seen one person shun their responsibilities.
Are we scared, anxious, worried, concerned, stressed? We certainly are. Not as much for ourselves as for our families and patients. That said, we are charging forward and making a difference that will not be realized until we look back and realize what has been accomplished.
What do you think will be the long-term impact of this on the frontline healthcare workers?
I do believe there will be long lasting effects on the mental health of some of our providers. I believe that will make us look much more closely at a problem that has been overlooked for as long as medicine has been a profession.
Are health care workers equipped with enough PPE (personal protective equipment) and other supplies?
The short answer is no, but we have adapted to a new normal and are wearing PPE in ways that we have not done so before. Typically, PPE is one time use and we throw away everything. We are now re-using surgical facemasks, N95 respirators and face shields. We are still throwing away gowns and gloves. We are trusting the guidance of the CDC and WHO that this is a safe practice and doing what we can to protect ourselves. Should this prove to be inadequate, we will certainly find out as more and more health care providers become ill with COVID-19.
I could not be more proud of a country that has come together to take care of those of us on the front line in this manner.
I am protecting myself, and certainly more aware when I am in clinic, washing my hands incessantly and using hand sanitizer before and after every patient (and generally every time I feel like five minutes have passed and I haven’t put any on.)
As I and most of my colleagues see it, I have two choices. I can refuse to see patients, or I can protect myself the best I can and do what I do every day. PPE is becoming more available daily, and supplies are being donated by average citizens and companies hourly. I could not be more proud of a country that has come together to take care of those of us on the front line in this manner.
Are we making any progress in “flattening the curve?” Can you help readers understand what this means and how it will help stem the spread of the virus?
Flattening the curve is a term that essentially means slowing the spread of the virus to make the situation manageable. We can’t stop the virus, but what we can do, primarily by physical distancing, is decrease the rate at which people spread the virus to each other.
Although it may not reduce the total number of people eventually infected, it will spread that number over several weeks to months allowing the health care system time and equipment to deal with the numbers.
This is a critical moment.
Over the last couple of days, we are seeing a reduction in deaths in NYC. This hopefully means we have reached a peak and that we are on a downward trajectory.
This is a critical moment.
If people continue physical distancing and preventative measures such as wearing masks and gloves when they do have to go out, positive trends will continue. The risk is that people will see positive indicators as a sign that they can return to normal, and we will see a rapid return to crisis. I am grateful that most people are taking this very seriously and are truly contributing to mitigating the impact this will have in our states.
What’s the status on testing? Why is it taking so long?
The U.S. government must protect its citizens. There is clearly an intense and urgent need for better testing, treatments, and information. However, it is, and will continue to be in the best interest of our country to maintain a strict protocol for approval of treatments and testing. The Food and Drug Administration (FDA) has the very important task of ensuring that any test or treatment that is approved for use in the U.S. has been extensively tested and found to be safe and effective.
It is, and will continue to be in the best interest of our country to maintain a strict protocol for approval of treatments and testing.
During times of crisis, such as this outbreak, or the recent Ebola crisis, the FDA can make products or drugs available under emergency use authorizations. This is not the best way to work.
If a test is approved too hastily, there is a high risk of ineffectiveness, often in the form of “false negative” results. This means people could take the test and have a negative result, but actually be infected and contagious. This could be devastating, especially with the aggressive COVID-19 virus where we see individuals being infected for several days before showing symptoms.
Every health care provider would love to test every patient. For now, it is better to wait for more effective tests, continue self-quarantine, and treat everyone with symptoms as if they are infected.
Through the lens of this pandemic, what are you finding to be the strengths of the healthcare system? Regionally? Nationally?
Regionally, being hit much later than many countries and states, gave us the ability to plan and prepare far better than other areas that have been harder hit. Both Rhode Island and Massachusetts were more proactive in taking measures to minimize the health care impact of this outbreak. We mobilized medical resources in record time. Our hospital systems conduct drills and prepare for mass casualty events, and our providers maintain proficiency in infrequently used skills.
On a national level, our incident command structure has stood the test of time and events. The national stockpile allows for the quick provision of supplies to areas of critical need. Our military, especially our military medical providers, are extensively trained to work with little information and guidance, often in hostile and austere environments, and thus, are able to be deployed expeditiously to the areas of greatest need and make an impact almost immediately.
The resources and ingenuity of [scientists, researchers, clinicians, etc.] cannot be underestimated.
In New York City, for example, the National Guard, followed by active duty military members, were on the ground almost immediately, and the Army Corp of Engineers were able to construct field hospitals within days. Also, the USNS Comfort and the military are providing almost 3500 additional beds along with expert providers and the best equipment to a stressed medical system. If a military provider has not seen or dealt with a situation in the past, just give them a day or two, and they will have found a means to make it work.
Our scientists, researchers, clinicians, and facilities are working tirelessly to find cures, treatments, vaccines, and other measures to combat this virus. The resources and ingenuity of this group cannot be underestimated. Information is being shared in real time across the world and guidelines and protocols are being updated almost instantaneously. The ability to share so much data in real time is improving care as I write this.
Where are the weaknesses?
Some of the things that stand out are the limits of our supply chains, especially when they are tied to other affected areas. Our lack of contingency beds and supplies has proven to be a significant rate limiting factor. More weaknesses will come to light over the next several months and years.
The federal government and the states need to have better systems in place to deal with future incidents.
As we moved away from massive stockpiles of supplies in hospitals to a system of “just-in-time” ordering, we assumed that manufacturing was limitless. This did not take into account a worldwide pandemic. The military, which continues to have stockpiles, has already proven this to be the case. There will have to be some balance established. We cannot, and should not, stock unreasonable amounts of equipment that may never be used. It may prove better to have a contingency for creating it more efficiently and effectively in a time of need. Many of our hospitals run on very narrow margins and cannot afford to keep unlimited staff, supplies, and beds for a “what-if” situation. The federal government and the states need to have better systems in place to deal with future incidents. We will not be able to afford trillions of dollars should such pandemics recur.
Why was the system not well-prepared for this crisis?
The last worldwide pandemic was 1918. I think we were as prepared as we could be for this event. There will be blame thrown around for this for the next several years. The health care system is a business like every other business and must look at making investments that are healthy for the future of their organization. It would not be cost effective to plan for contingencies at the expense of being able to provide the day-to-day services needed to treat patients and prevent disease. Although we have learned so much from this particular pandemic, we cannot know what the next disaster will bring. Our next worldwide event may not be viral and may not overwhelm our healthcare system in the same way. That being said, bed shortages, manufacturing capabilities, and staff shortages should all be looked at very carefully.
What are we learning now to better prepare for similar situations, which seem likely?
Though some of what we are learning is specific to this virus and this pandemic, the lessons for broader, long-term application are in the areas of skills, diplomacy, and the ability to work together as a global community to understand what it takes to overcome a worldwide catastrophic event.
We are learning how such events can impact every aspect of our lives—social, psychological, and financial.
We are learning how such events can impact every aspect of our lives, social, psychological, and financial. These lessons will need to be studied at length to determine how we can best anticipate and manage future events.
We are also seeing so much misinformation and even conspiracy theories surrounding this pandemic. Ethically challenged individuals are using this for financial gain by scaring people or charging outrageous prices for goods and services. Not only can you not find a roll of toilet paper in the grocery store, but I have seen web cameras selling for hundreds of dollars and N95 respirators being sold for thousands of dollars a box. Every day I spend hours trying to debunk myths, hyperbole, and outright lies on the internet. Even the major news networks, vying for viewers and ratings, are sensationalizing the news and often inducing unnecessary panic. I am fully supportive of free speech and do not suggest any form of censorship, but encourage those who are knowledgeable to speak up and correct inaccuracies as they are found.
It is almost certain that we will see this virus return next winter. Our best bet for getting ahead of this virus and managing the next outbreak will be a vaccine. The likelihood of a successful vaccine being approved and generally available before next winter is low. Because of this, we need to be prepared to undertake intense contact tracing, a process by which we identify every person a sick person has been in contact with and investigate them. We will still have to practice significant physical distancing, but we can do it in a much more focused manner based on these investigations. Another country-wide restriction on activity would be devastating to our economy.
Stay the course.
What would you say to people who ask how they can help?
The best ways to help are to follow physical distancing rules and stay home as much as possible. A note about the difference between physical and social distancing. Please enjoy as much social interaction as possible, just make sure it’s virtual – by phone, computer, social media, etc. Other suggestions include:
-
Stay the course. Please, please don’t jump right back in once the numbers start looking better. It’s going to take time. Be patient. Follow your leaders’ guidelines. They want to get things running again just like all of us, but they see the bigger picture.
-
Check in (virtually) on the vulnerable members of your community. Our elderly, infirm, socially isolated, depressed, anxious, and substance abuse patients are all lacking the very needed social interaction that is keeping them alive and healthy. It has never been more important for providers to check on their vulnerable patients, and for neighbors and friends to check on their friends and loved ones.
-
Get vaccinated against the flu and other communicable diseases. When a vaccine becomes available for this virus, get it as soon as possible. Herd immunity works and will prevent subsequent outbreaks of this very virus.
-
Please educate yourselves on the facts. It can be confusing because the circumstances are changing fast. When in doubt, get your information from the CDC and WHO websites, and reputable news sources. Avoid unsourced and unverified social media content. If something doesn’t seem right, it probably isn’t.
-
Give blood! With all the physical distancing, people are not giving blood and hospitals across the country are facing critical shortages.
-
Thank your local health care providers. Consider dropping off coffee, donuts, food, or something like that. As much as we love that people are making homemade masks, we likely cannot use them in the hospital. A few examples of helpful items to donate are stethoscope covers, headbands, surgical caps, goggles, etc. These are great thing to donate to your local health care facilities.
What are you most thankful for?
I am glad for all of the people in my lives both personally and professionally who have reached out to check on me and show their appreciation. I want to thank those on the front lines, the behind the scenes folks who make my job possible. Never have I been more grateful for the environmental service people who are making my environment safe to work in; the front desk staff who are triaging people with little information, and are wearing PPE having never done so; the people who are still serving food in the cafeteria while we are patiently waiting six feet apart in line; the teachers and day care providers who are caring for our children so we can go to work; the endless number of people keeping our grocery stores stocked and open; and the EMTs, Firefighters, Police Officers, and security guards who are making sure our patients are getting the best care they can from the very beginning, often without the security provided in the hospital.
We will all come through this pandemic better because we are working together and committed to the common good. Be safe and be healthy!